15% off £30 OR 20% off £40
What is eczema and how do I treat it?
.png)
The word eczema comes from the Greek word ‘ekzein’, which means ‘to boil out.’ Believe it or not, it’s one of the most common skin conditions you can have, with one in five children and one in 20 adults having the condition.
But you don’t have to put up with eczema, there’s lots you can do to ease your symptoms.
What is eczema?
Eczema is an inflammatory skin condition that triggers dry, itchy skin and skin rashes. Also known as dermatitis, eczema affects five million people in the UK each year.
You can develop eczema symptoms at any age, although it’s more common in children. Most people grow out of it, although some may continue to have dry skin or be prone to flare-ups later in life.
The most common type of eczema is atopic dermatitis, but there are many other different types, including irritant dermatitis, allergic contact dermatitis, dyshidrotic eczema, nummular eczema and seborrheic eczema, also known as Cradle Cap.
Is all dry skin eczema?
A quick distinction. Not all dry skin is eczema. Dry skin is a skin type (oily, combination and normal are others), and there are times when we can all expect our skin to show signs of lacking moisture. For example, cold weather, harsh chemicals and excessive hand washing can all damage the outer skin and cause dry skin to form. It often shows up as patches of flakiness and in extreme cases, cracking.
On the other hand, eczema is a chronic, inflammatory skin condition. It often flares up sporadically, leaving sufferers with red, dry, itchy skin. And not just a little tickle of an itch, it’s a type of irritation that’s hard not to scratch.
The exact cause of eczema is debatable, but in general terms, it’s down to a response by your immune system to… something. To what? Well, there are a whole range of things that could be triggers. A skincare product you’ve applied to your skin. Or a new detergent you’ve used to wash your clothes. Maybe dust, pollen or another allergen in the environments. Something you’ve eaten. Eczema can also be exacerbated if you’re feeling under the weather. And the most annoying thing is, it can be difficult to find the underlying cause.
Common types of eczema
The two most common types of eczema are:
-
Atopic eczema
Is caused by a combination of genes and environmental factors. Symptoms of atopic eczema include red, dry, scaly patches and skin rashes that itch.
It can occur anywhere, but is most often seen in skin creases, such as the backs of the knees. It’s also possible to get atopic hand eczema and for it to also develop on people’s feet. During flare ups, skin can weep, crust and bleed. Further complications, such as infections, may develop, especially if you have severe eczema.
What causes atopic eczema?
In healthy skin, fats and oils made by your skin seal in moisture – plumping up skin cells with water – so the skin’s outer layer becomes a barrier against infection and irritation.1
However, if you have atopic eczema, your skin makes fewer fats and oils than it needs to stay healthy. The latest theory is that it’s caused by a particular gene mutation, which triggers a deficiency of a protein called filaggrin – needed for skin cells to hang on to water.2 Without this, not only does the skin lose vital moisture, but gaps emerge between previously plumped skin cells – like losing mortar around the bricks in a wall – allowing infections and irritants to enter.
Soap, shampoo, shower gels and other everyday substances can then start to dry, irritate and inflame skin. And dry, damaged skin is highly susceptible to sensitisation by allergens.3
-
Contact dermatitis
Causes a localised reaction to take place, which results in redness, itching and burning where the skin has been in contact with an allergen or irritant, such as acid, cleaning products or cosmetics. Contact dermatitis accounts for 84 to 90% of work-related skin disease.
Other types of eczema include seborrheic, which affects the scalp; and discoid, which causes coin-shaped patches of eczema on the body.
What are the symptoms of eczema?
All of the different types of eczema have the same symptoms, but your doctor will be able to tell you from your eczema symptoms, which particular strain you have.
Eczema can cause the creases in your arms and legs to become dry, itchy, cracked, scaly and red. If you scratch the affected skin, then it can grow thicker and split.
If your eczema becomes infected then you can get painful blisters full of pus and lumps that weep, bleed and crust over. You can also get eczema on your face, neck, as well as scalp eczema, and eczema over other parts of your body.
Severe eczema can keep you up at night, making it difficult to get the recommended eight hours of sleep because you feel so itchy. This can impact on both your personal and work life as you’re likely to feel drained and tired most of the time.
Common eczema triggers
In eczema, the skin is less able to retain water within its cells and to produce fats and oils. This means the skin’s barrier function is compromised, leaving it susceptible to dryness, irritation and infection.
There are lots of different things that can result in you developing eczema. Some of the main eczema causes are:
- Having a food allergy/intolerance
- Your genetics – some types of eczema are hereditary
- Having asthma
- Using harsh soaps and skincare products that irritate your skin
- Your body producing more of the IgE antibody than needed, which can impact your immune system
- Having a viral infection
- Your skin not forming a strong enough barrier
- Having an allergy to dust mites, pollen, cats or dogs
- Being stressed
- Having other medical conditions
- Being in close contact with chemicals and irritants at work or in the home, without wearing protective gloves or clothing
- Changes in the weather. Cold spells can dry your skin out, making you more prone to eczema
Who is most likely to get eczema?
Atopic eczema often affects young children, but most grow out of it before they become teenagers.
However, a tendency develop to atopic conditions, including eczema, hay fever or food allergy, often runs in families.
Some adults are prone to atopic eczema too, particularly if they use irritant chemicals in their job, such as hairdressing, cleaning or nursing.4
How to treat eczema
There are a few different ways to treat eczema and relieve its symptoms.
Baby eczema
It’s not uncommon for red, dry or itchy skin patches to develop on a baby’s face, behind their ears and/or within the folds that are on their neck, knees and elbows. (5)
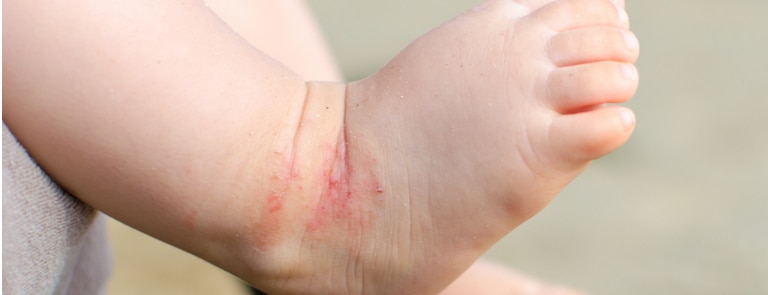

Baby eczema is something that most babies grow out of as they get older however, in the meantime, they may scratch at their eczema patches, which could result in them getting infected.6 Interestingly, baby eczema can flare up if they’re feeling under the weather, e.g. they’re teething, have a cold or are overtired.7
Treatments and prevention tips for baby eczema are varied and include: using unperfumed moisturisers on the eczema patches, avoiding aqueous cream, as this can cause burn and sting the skin, and dressing your baby in light, cotton fabrics.8
Eczema in children
Almost three in four children who experience eczema will find that it clears up by the time they’re seven-years-old.
.jpg)
.jpg)
Atopic eczema is more common in children and often develops before they turn 1.9
Children who have eczema, usually tend to develop it in the folds of their elbows and/or knees. It can sometimes appear on their hands – at least 70% of people have had hand eczema at some point in their life.
Redness and itchy patches behind children’s ears, on their feet or scalp, may also be a sign of atopic dermatitis. They could also be symptoms of other conditions, such as seborrheic dermatitis, which can exist with eczema.10
Treatment for eczema in children is very similar to treatment for baby eczema.
Adult eczema
Adults also tend to develop atopic dermatitis on different parts of their bodies to children.
These areas include the backs of their knees, back of their neck and around their eyes. The skin around the eyes can also become extremely itchy.


Some people may live with eczema for many years however, the right eczema treatments can make it manageable.
Your GP may refer you for allergy testing to identify any causes. They might recommend soap substitutes or prescribing you antibiotics or antihistamines.
How to avoid symptoms of eczema
If you live with eczema, you may have realised that certain things can trigger a flare up. Make sure you keep a note of your triggers. In the meantime, make sure you:
- Avoid products that could irritate your skin
- Nourish your skin with a moisturiser
- Keep a note of different foods that trigger your eczema and then eliminate them from your diet
- Drink plenty of water and follow a diet that’s filled with fruit, veg and essential fatty acids
Tips to prevent an eczema flare-up
While you can’t fix a family tendency to develop eczema, you can make some changes to help support your skin and reduce the risk of a flare-up:
1. Moisturise your skin with emollients
Moisturise your skin with emollients – these contain a mixture of fat and water.


Choose shower or bath emollient and a moisturiser-style emollient, either as a cream, lotion or ointment. Rub it in after bathing, when your skin is still damp, to lock in moisture.11
2. Keep a diary to work out triggers
It's important to know what can set off your eczema, so noting down what you were doing before a flare-up can be helpful.


Common triggers can include12:
- cigarette smoke
- stress
- change in temperature
- dust mites
- pet dander
3. Eat oily fish
A 2016 review in Dermatology Practical & Conceptual found that taking omega-3 fatty acids (found in oily fish such as mackerel, tuna, herring and salmon) improved eczema symptoms overall,


Omega-3 also helped to decrease the size of rashes.13 However, the researchers suggested more studies are needed.
In addition, eating oily fish or taking fish oil supplements in pregnancy may reduce the risk of your baby developing eczema, according to a 2017 study by University of Southampton.14
Always speak to your midwife or GP before taking any dietary supplements while pregnant.
4. Consider using plant oils
A 2018 Taiwanese review found that jojoba oil, rosehip oil and oat oil (found in colloidal oatmeal) all have anti-inflammatory effects on eczema.


Researchers also reported that oatmeal can help support skin barrier repair.15
Managing your eczema symptoms
If your eczema is severe then you shouldn’t suffer in silence. Go and speak to your doctor as they can prescribe steroid eczema creams or other ointments for severe eczema.
For atopic eczema, emollients (moisturisers) need to be used every day and topical corticosteroids (topical steroids) creams and ointments should be applied during flare-ups.
Depending on the severity of your eczema, your doctor might refer you to a dermatologist who can put together a tailored eczema plan. They might suggest phototherapy (light therapy) and/or stronger medication.
Last updated: 11 March 2021
- https://eczema.org/information-and-advice/our-skin-and-eczema/
- https://nationaleczema.org/skin-directed-atopic-dermatitis-report/
- https://eczema.org/information-and-advice/our-skin-and-eczema/
- https://knowyourskin.britishskinfoundation.org.uk/condition/eczema/
- https://www.nhs.uk/conditions/pregnancy-and-baby/eczema-in-children/
- https://www.nhs.uk/conditions/pregnancy-and-baby/eczema-in-children/
- https://www.nhs.uk/conditions/pregnancy-and-baby/eczema-in-children/
- https://www.babycentre.co.uk/a541297/baby-eczema-causes-symptoms-treatments-and-creams
- https://www.nhs.uk/conditions/atopic-eczema/
- https://nationaleczema.org/eczema/children/
- https://eczema.org/information-and-advice/treatments-for-eczema/emollients/
- https://nationaleczema.org/eczema/causes-and-triggers-of-eczema/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5006549/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5537898/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5796020/













